Services
Home / Services
Importance of Routine Eye Exams
Ophthalmology Services
For Albany, Schenectady, & Saratoga Springs, NY
They say “you are only as good as your tools” and when it comes to your eyes, our office has spared no expense. As comprehensive eye physicians, surgeons & cornea specialists, we provide a number of ophthalmology services for the people of Albany, Schenectady, Troy, Saratoga Springs, NY and the surrounding areas. Our eye doctors utilize only the best and most modern equipment for the assessment and maintenance of your vision, representing the gold standards in medicine and eye testing technology. We proudly offer a wide variety of tests that can be performed during your office visit for your convenience.
Contact us today to schedule your appointment with an ophthalmologist at our office.
Our Ophthalmologists Value Proper Education
At our office, we greatly value patient education. We believe a well-informed patient is not only a more proactive patient in his or her eye health, but is also a happier and healthier patient. As such, we would like to take a few minutes of your time so that you can better understand your own eye health and what is required to maintain optimum vision for a lifetime. Here, you will learn about some common eye conditions that you may experience in your lifetime. We also invite you to check out our educational videos so you can become familiar with common conditions.
Our Ophthalmology Services Include:
A Below are comprehensive explanations of the services and treatments we offer. To go directly to a specific service or treatment, click on a service or treatment below. If you are having issues with your vision, please give us a call. We will bring you in for an appointment and provide you with the necessary treatments.
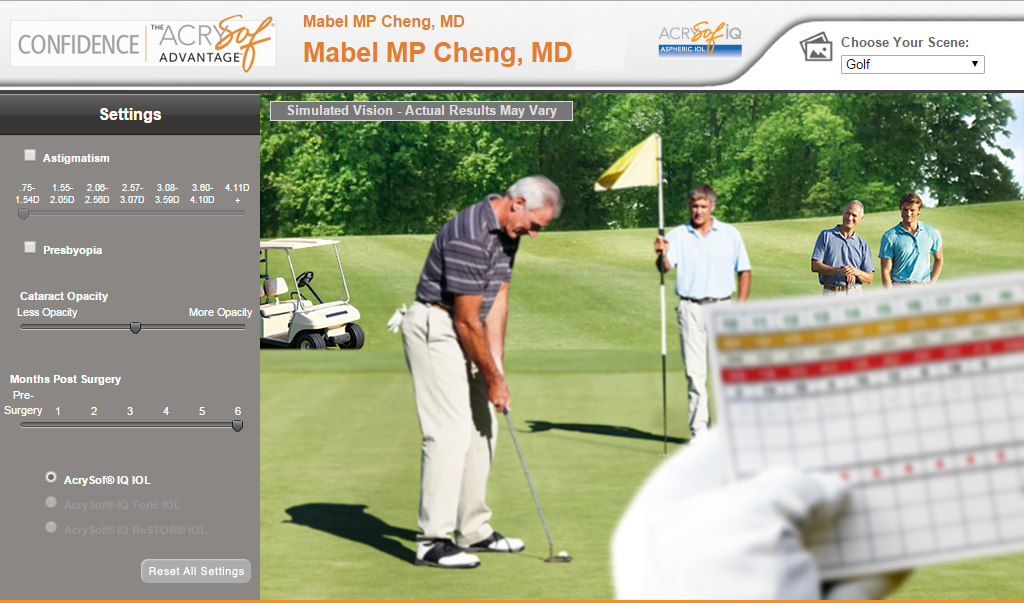
Treatment Spotlight: Cataracts
In cataract surgery there are a couple of different options that you have. There are many lenses out there that allow you to get the vision that you want. Watch this video featuring our practice administrator, Brian Lemanski, as he explains the different options available and goes through in details the different types of cataract treatments.
Eye Exams Offered Throughout Albany, Schenectady & Saratoga Springs, NY
Dr. Mabel Cheng and Dr. Nicole Lemanski, is proud to offer most state of the art imaging test for eye exams throughout Albany, Saratoga Springs and Schenectady, NY. Take a look at some of the testing that we offer to our patients. Scroll over each box below to learn more about each test and how we conduct them at the office. During an eye exam, our ophthalmologist uses a wide variety of tests, including the ones featured below, to properly test your eyes for any problems and then properly treat any issues discovered. If you have any additional questions on our tests, don’t hesitate to give us a call!

Visual Acuity Assessment
A non-invasive test that examines how well you can see up close and far away.
VISUAL ACUITY ASSESSMENT
In some instances, this is done for legal purposes such as determining if a patient is fit to drive a car. This 5-minute test is generally accomplished by looking at a chart containing letters of different sizes and reading the letters back to a technician.

Refractions
An extension of a visual acuity test.
REFRACTIONS
This non-invasive test, performed manually or with a machine, determines the strength of the corrective lenses (glasses) or contacts that are needed for you to see clearly.
Wavefront Abberometry
Mapping the unique visual 'fingerprint' of how your eye bends light.
WAVEFRONT ABBEROMETRY
Using the same shack-hartmann technology utilized by NASA in its space telescopes, our wavefront aberrometer allows us to examine the unique properties of how your eye bends light. This information is then used for numerous purposes, from determining candidacy for LASIK or premium multifocal lenses for cataract surgery, to making highly accurate corrective lenses (glasses).

Meibomian Gland Imaging
A means of visualizing the meibomian glands, the glands that produce oil to keep your tears from evaporating away.
MEIBOMIAN GLAND IMAGING
Our eyes produce tears to lubricate the eye. However, in order for them to remain on the ocular surface, they require protection from evaporation. The Meibomian Glands, located in your lids, produce oil that prevent tear film evaporation. In some cases, the Meibomian Glands become clogged meaning oil cannot get to the ocular surface. Left untreated, these clogged oil glands will lead to permanent gland loss. Since these glands cannot be fully visualized by human eyes, we are proud to introduce this special camera to our office for the benefit of our patients for early detection of Meibomian Gland Dysfunction.

Tear Lab Tear Osmolarity Test
The tear osmolarity test is used to measure the composition of your eye’s tears.
TEAR LAB TEAR OSMOLARITY TEST
The results of this test give insights into whether the tears you produce are good enough to lubricate the cornea. Poor tears or not enough tears result in Dry Eye Disease. This test takes roughly 2 minutes to complete. During this time, a technician will obtain a small sample of your tears from the corner of your eye and analyze it in the Tearlab machine.
Visual Field (VF) Test
A non-invasive test that examines a patient's central and peripheral field of view.
VISUAL FIELD (VF) TEST
The results from this test notify the eye physician of any significant changes the patient has in their field of view. These data are very useful in the early diagnosis and monitoring of, glaucoma patients, macular degeneration patients, patients that have received trauma to the eye, as well as patients on certain drugs that may be toxic to the eye (e.g. plaquanil).
During the test, the patient will sit and stare at a fixed point within the analyzer. The analyzer will then flash a series of lights in various places while the patient clicks a button to indicate that he / she has seen the flash.

Optical Coherence Tomography (OCT)
A non-invasive test that utilizes light to examine the different layers of tissue in the retina.
OPTICAL COHERENCE TOMOGRAPHY (OCT)
By measuring the thickness of these tissues, eye physicians can better detect, diagnose, and treat certain retinal (or corneal) diseases, especially macular degeneration and diabetic retinopathy. It is also useful in assessing the health of the optic nerve, which may be damaged by diseases such as glaucoma.The test is generally conducted while dilated and takes a few minutes to complete. During that time, the patient sits and stares at a fixed point while the OCT scans the eye. The procedure is then repeated for the other eye.

Endothelial Cell Count
A means by which the number of corneal endothelial cells are quantified.
ENDOTHELIAL CELL COUNT
We are all born with a fixed number of corneal endothelial cells which naturally die over time and are not replaced. However, trauma and certain eye diseases, such as glaucoma and uveitis, can accelerate the loss of these cells, potentially necessitating a corneal transplant. By quantifying these cells, eye physicians can track the status of the endothelium and be better able to detect and treat ailments before irreversible damage occurs.
This non-invasive test takes roughly 3 minutes to complete. During this time, the patient will sit down and stare at a fixed point while the cell counter images the eye via a flash photo. The procedure is then repeated for the other eye.

Anterior Segment Tomography
High Resolution, 3-D reconstruction of the front of the eye.
ANTERIOR SEGMENT TOMOGRAPHY
A non-invasive means by which a 3-D reconstruction of the front of the eye is be generated and analyzed for diseases of the front of the eye, such as Keratoconus. Results from this test can also be used to examine the thickness of the cornea, needed for accurate Tonometry, as well as examine refractive errors, such as astigmatism, with high resolution for specialized glasses, contact lens fits or LASIK evaluations.
This test takes roughly 5 minutes to complete. During this time, the patient will sit down and stare at a red/blue dot while a camera rotates around the eye.

Ultra-WideField Fundus Photography
A non-invasive way to image large portions of the retina for future comparison.
ULTRA-WIDEFIELD FUNDUS PHOTOGRAPHY
While most cameras can only image 45 degrees of the retina, our confocal scanning laser ophthalmoscope can image 200 degrees, allowing our physicians to see into the periphery of the retina where pathology can go unnoticed. Our camera can also perform auto-fluorescence imaging to examine damage to the retina as well as fluorescein angiography to visualize blood vessels.
This test takes 5 minutes to complete. For this test, the patient will sit in front of the camera and view a target that will change color when the eye is properly focused. A flash of light will be then seen during image capture.

Non-Contact Comprehensive Biometry
A touch-free method to assess four different parameters that are critical for good cataract surgery outcomes.
NON-CONTACT COMPREHENSIVE BIOMETRY
These include measuring how long the eye is, how physically big the eye is, what the curvature of your cornea is, and how deep the area from your iris to your cornea is. This data, measured to the hundredth of a millimeter (or one tenth of a thousandth of an inch), is then statistically analyzed against advanced mathematical formulas that help determine the strength of your lens implant. Measurements taken here can allow most patients to enjoy freedom from glasses after their cataract surgery, should the patient desire.
This test takes roughly 5 minutes to complete. During this time, patients will be asked to fixate on a light while the device analyzes all four parameters. The test is then repeated on the other eye.

Quantitative Pupillometry
A highly reproducable, objective, and quantitiative approach to screening for afferent pupillary defects, or APDS, caused by asymmetric retinal or optic nerve disease.
Quantitative Pupillometry
The classic way of screening for afferent pupillary defects, or APDs, involves holding a penlight to one eye and watching the pupil response in the other. When one eye responds to light differently, it can be a sign of damage to the retina / optic nerve. This test, when performed manually, is difficult to accurately perform, relatively insensitive, and is highly variable between observers. The introduction of quantitative pupillometry, a first in the Capital Region, allows us to perform a much more sensitive and objective evaluation.
This test takes roughly 1 minute to complete. During this time, patients will be asked to fixate on a target while the device flashes light at one eye at a time. The test is then repeated on the other eye.